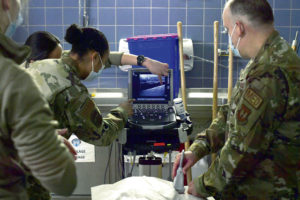
The 86th Medical Group Ground Surgical Teams sharpened their skills during a training at Landstuhl Regional Medical Center, Feb. 9.
The training included simulated patient scenarios and specific skill stations, in which two teams exercised emergency medical and surgical care similar to that encountered in a deployed environment.
“Trainings like this are important to develop motor memory,” said Lt. Col. James Spencer, 86th Medical Squadron nurse anesthetist. “Whenever you’re in a battlefield situation, and you’re receiving incoming patients that are hurt really badly, sometimes that adrenaline makes it difficult to think. This process keeps us focused, actually helps get rid of some of the fog of war and allows us to think clearly and systematically.”
A GST provides damage control surgery, damage control resuscitation and emergency care of injured or critically ill patients in dynamic, austere environments outside of established support and patient movement capabilities.
“Our team is designed to take care of a patient that requires what we call damage control surgery, which is usually an injury that is not amenable to a tourniquet,” Spencer said. “Using our team and our resources, we can first diagnose where the bleeding is coming from and not only resuscitate the patient, but also open the abdomen, chest or wherever the bleeding is coming from, and hopefully stop that bleeding so the patient can make it to the next level of care.”
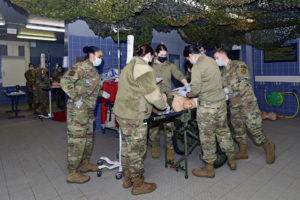
With their primary mission being to stabilize and prepare patients for casualty evacuation, GSTs are skilled in multi-system trauma, blunt and penetrating trauma, shock and hemorrhage control, respiratory and airway management, management of thermal injuries, limb revascularization, stabilization of fractures and major wound debridement.
Each team is composed of an anesthesiologist, clinical nurse, emergency services physician, general surgeon, health services administrator and surgical services craftsman. When oncall, a team must be ready to deploy with a six-hour notice.
“I think the most important thing today was probably the team dynamics,” said Maj. Katherine Cameron, 86th Medical Squadron general surgeon. “We don’t always get to work, just us, in the operating room and in the emergency room at (LRMC) since we’re a joint hospital. It’s always good for us, for our team dynamics, to get to simulate and work together, since we’re the ones that would be going together for any missions.”
Training exercise stations were also used to provide GST members with demonstrations and the chance to hone specific skills.
“We did some targeted skill stations for practice, such as arterial line placement and central line placement,” Cameron said.
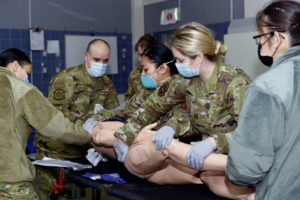
Being the smallest deployable Air Force module for delivery of advanced emergency patient care, GSTs perform trauma-focused training at least one week each month during their call period to remain proficient and capable.
“I hope the takeaway is, whenever we’re actually in the field, and we’re receiving that patient that’s injured, we can remember our processes, fall back on our training, take care of that patient, and do the best we can for them,” Spencer said.
The teams’ dedication to enhanced performance ensures they are ready to execute downrange patient stabilization and secure patient survival to the next level of medical care.


