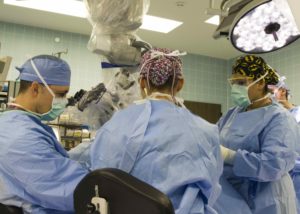
Over the span of two weeks, Landstuhl Regional Medical Center’s Ear, Nose and Throat Clinic maximized on the opportunity to provide specialized ear treatments to troops from Europe and Africa, their families, and military retirees, during LRMC’s Ear Week, Nov. 13-24.
During the 11-day Ear Week, patients in need of specialized ear procedures were scheduled for surgical interventions with U.S. Army Maj. Douglas Ruhl, a visiting otologist assigned to the 53rd Head and Neck Team with the 47th Combat Support Hospital, based out of Joint Base Lewis-McChord, Washington.
While Ruhl is assigned to a U.S. Army Forces Command unit, he practices at Madigan Army Medical Center at JBLM as part of the Army’s Modified Table of Organization and Equipment Assigned Personnel, which allows medical professionals to become an organic part of a deployable unit while maintaining their place of duty at a U.S. Army Medical Command Military Treatment Facility.
“(Ear Week) lets me do more cases in a short period of time than I would normally, which is nice for me since I wear two hats,” said Ruhl, who completed a two-year neurotology fellowship at the University of Virginia. “I get to help medical and combat readiness and I get to dabble in the different roles of care so it works out well.”
During Ear Week, ENT staff operated in a similar fashion to medical residencies, maximizing caseload and supplementing specialists while operating within appropriate levels of expertise.
“One of the reasons of having this ear week is to allow (LRMC ENT staff) to keep that skill set from completely atrophying, so we go in and kind of function in a way like we did in medical residency where we help with the surgery, and then when it gets to the point where it’s out of our expertise level, the otologist will take over,” said U. S. Air Force Maj. Whitney Pafford, otolaryngologist assigned to LRMC’s ENT Clinic.
Patients benefit from the specialized treatments without the need for referral to host-nation providers, which can further complicate a patient’s understanding of potential risks due to language barriers or treatment modalities.
“(The diagnosis are) not emergent, so patients don’t have to have surgery in a month and can wait three to five months to have surgery until a specialized provider comes out here to do it,” said Pafford. “There are some cases we’re all trained to do but unless you’re doing them regularly, (the procedures) are pretty specialized, requiring one to two years of fellowship.”
Additionally, because there are serious risks involved with the specialized surgical procedures, including worsening hearing, or damage to nerves, they are reserved for specialists who perform them on a regular basis. For military personnel, otologists may provide medical treatment to potentially career-ending diagnosis such as sensitivity to pressure changes or loss of hearing.
Aside from making specialized ear procedures available for beneficiaries, waiting until Ear Week also allows patients to follow up with LRMC providers and is cost-effective for the Army.
“Instead of just sending every procedure out to (host-nation specialists), hosting (Ruhl) is beneficial because the amount of money it takes to bring him out here is a fraction of what it would be for one person’s surgery,” said Pafford. “Ear surgery is pretty expensive, especially once you go to the more complex ear surgeries.”
According to Pafford, if patients are in dire need of surgery, such as when diagnosed with acoustic neuroma, or a patient doesn’t want to wait for Ear Week, they can be sent back to the continental United States for their procedure where they’ll stay during post-operative care until it’s safe to fly back. This could take up to four weeks due to risks associated with high altitudes following surgery.
Although the objective of this partnership with FORSCOM is to equip deploying units with qualified health care professionals, providing care at LRMC benefits all unified combatant commands overseas.


